What is laparoscopy?
Examination of abdominal cavity and its contents with the help of a telescope is called as laparoscopy. A complete examination of a woman’s internal pelvic and abdominal structures can provide important information regarding infertility and commom gynecologic disorders. Frequently, problems that cannot be discovered by external physical examination or ultrasound can be discovered by laparoscopy or hysteroscopy, two procedures which provide a direct look at pelvic and abdominal organs.
What is diagnostic laparoscopy?
When laparoscopy is performed for the purpose of diagnosing a disease in a patient, it is called diagnostic laparoscopy. laparoscopyis useful in diagnosing many gynecological problems including endometriosis, uterine fibroids and other structural abnormalities, ovarian cysts, adhesions, and ectopic pregnancy. Laparoscopy and hysteroscopy together is the gold standard in the complete evaluation of infertile female.
When diagnostic laparoscopy is performed in relation to menses?
Generally, the procedure is performed after the basic infertility tests, although the presence of pain, the history of a past infection or the other problems diagnosed on physical examination or ultrasound may indicate a need to perform diagnostic laparoscopy sooner in the evaluation. The procedure is usually performed after menses in case a hysteroscopy is also necessary. The uterine cavity is more easily evaluated after menses and there is little risk of interrupting a pregnancy. After the medical history, which consists of questions about the patients previous illnesses, treatment taken, menstrual cycle pattern, etc and physical examination are completed, laparoscopy is usually performed on an outpatient basis, under general anesthesia with minimal discomfort.
How laparoscopy is performed?
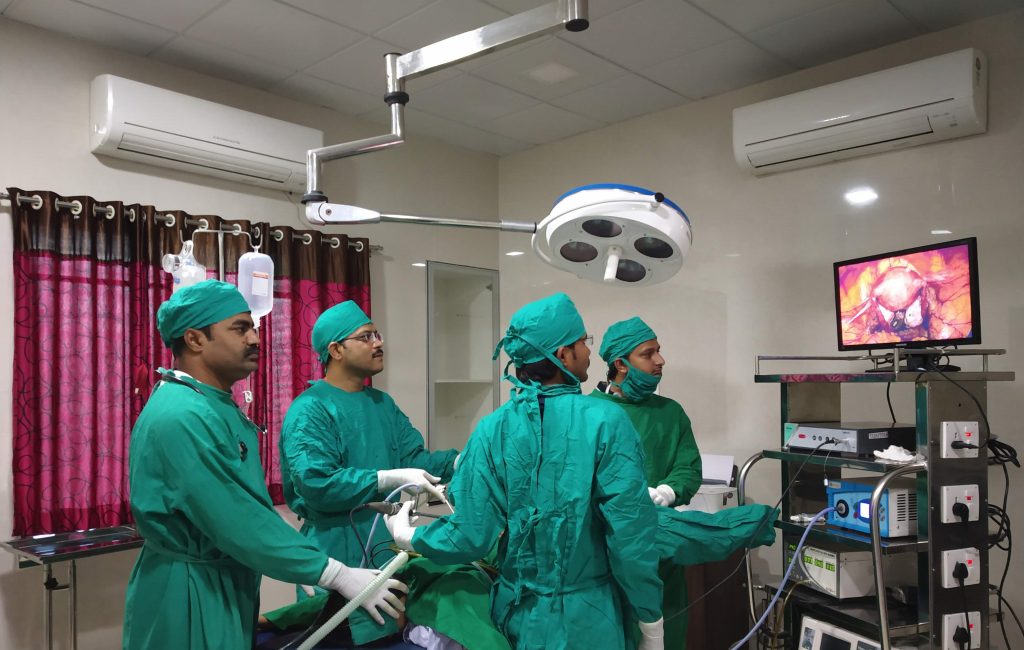
After giving general anesthesia, a 5mm or 10 mm port is inserted through or near the umbilicus and the abdomen is filled with carbon dioxide gas. The gas pushes the internal organs away from the abdominal wall so that the laparoscope can be placed safely into the abdominal cavity to avoid injury to surrounding organs such as the bowel, bladder and blood vessels. The laparoscope is a long, thin, lighted telescope like instrument that is inserted through the port. Video camera and light source is then attached to the laparoscope and the live picture of abdominal cavity wherever the camera is focused is seen on the monitor. The laparoscopic surgeon can see the reproductive organs including the uterus, fallopian tubes and ovaries. Another one to two small instruments (graspers) can be inserted through another 5mm port in order to move the pelvic or abdominal organs into clear view. To see the fallopian tube patency, a blue solution is instilled through the cervix, uterus and fallopian tubes. If abnormalities are detected, operative laparoscopy is performed in the same sitting.
What is operative laparoscopy?
When laparoscopy is performed for treating a disease, it is called operative laparoscopy. During operative laparoscopy many abdominal disorders can be safely treated at the same time that the diagnosis is made. While performing operative laparoscopy the laparoscopic surgeon inserts additional instruments such as probes, graspers, scissors, biopsy forceps, needle holders, electrosurgical or laser instruments through two or three 5 mm ports in the area above the pubic bone. The choice of technique and instrumentation depends on many factors including surgeon’s experience, location of the problem and availability of equipment.
Which diseases can be treated with operative laparoscopy?
Following diseases are treated with operative laparoscopy:
Opening of blocked fallopian tubes, removal of adhesions, endometriosis, ovarian cysts, uterine fibroids of any size and number, removal of ectopic pregnancy, removal of uterus (hysterectomy) for any cause, cancer surgeries of uterus, etc.
Reconstructive surgeries that can be done with operative laparoscopy: Tubal re-anastomosis after tubectomy operation, unification of two uteri (metroplasty), uterine sling surgeries for uterine prolapse, vault suspension surgeries, vaginoplasty, urogynecological surgeries, etc.
What postoperative care is to be taken after laparoscopy?
The patient is usually discharged on the same or following day after diagnostic or minor operative laparoscopy and on second or third day after major operative laparoscopy like hysterectomy. Patient can have liquids or light diet after six to eight hours after the procedure and can become ambulatory at the same time. Following laparoscopy, the umbilical area is usually tender and the abdomen may be bruised. Gas used to distend the abdomen may cause discomfort in the shoulders and abdomen. Anesthesia drugs can cause nausea and dizziness. The amount of discomfort depends on the type and extent of the procedure performed. Normal activities can usually be resumed within a few days. Significant abdominal pain, worsening nausea and vomiting, fever or significant bleeding from an incision requires immediate medical attention and hospitalization.
What are risks of laparoscopy?
Serious complications of diagnostic and operative laparoscopy are rare. Team of surgeons and anesthesiologists take all required care during and after anesthesia, surgery to prevent the complications. Also if complications arise, the team diagnoses and treats the complications efficiently. The major risk is damage to the bowel, bladder, ureters, uterus, major blood vessels, or other organs, which would require emergency surgery to repair. Injuries can occur during insertion of various instruments through the abdominal wall or during the operative treatment. There are other risks associated with laparoscopy, but they are all uncommon. Large hematomas of the abdominal wall can occur near the incisions. Pelvic or abdominal infections can occur. Allergic reactions, nerve damage and anesthesia complications rarely occur. Postoperative complications include urinary tract infection, skin incision infection, venous thrombosis, etc. When all possible complications are considered, one or two women out of every 100 may develop a complication, usually of a minor consequence. The risk of death during laparoscopy, which is about one to five per 100,000, is lesser than the risk of death during pregnancy. Certain conditions that may increase the risk of serious complications include: previous abdominal surgery especially bowel surgery, previous cesarean sections, severe endometriosis, pelvic infections, obesity, cardiorespiratory disease, etc.
What are disadvantages of open surgery?
Open surgery or laparotomy is generally performed through a bikini, transverse or vertical incision. Patients generally remain in the hospital for three to seven days following surgery and may return to the work in two to six weeks, depending upon the physical activity required. Nowadays many of the open surgeries can be performed by operative laparoscopy. Notwithstanding the advantages of operative laparoscopy, not all procedures can be performed with this technique. Some type of surgeries are too risky to perform laparoscopically, while in others it is not clear that laparoscopy yields as good as those by laparotomy. Finally the surgeon’s experience, skill also plays a significant role in deciding whether operative laparoscopy or laparotomy should be used.
What are the advantages of laparoscopy?
Putting it all together following are advantages
of laparoscopic surgery:
1.short hospital stay
2.less pain and fast recovery
3.cost effective
4.cosmetic surgery
5.less bleeding
6.early resumption to work
7.less infection rate
8.less chance of postoperative incisional hernia
Laparoscopy Procedures
- Diagnostic and Operative Laparoscopic Surgery
- PCO Drilling
- Total Laparoscopic Hysterectomy
- Myomectomy
- Metroplasty
- Sling Surgery for Uterine Prolapsed
- Ovarian Cystectomy
- Torsion Ovarian Cyst
- Ectopic Pregnancy Surgery
- Tuboplasty
- Tubal Ligation
- Vaginoplasty
- Appendisectomy